Cardinal Health MarketSM
The legacy Cardinal.com Medical Ordering site has been replaced with Cardinal Health MarketSM, a new product experience designed with you in mind.

04/27/2021
By Michele Holcomb, Chief Strategy and Business Development Officer at Cardinal Health
I lead a team that sets the course for the future of Cardinal Health. We look around corners, study the trends and drivers that will shape our industry and the competitive environment, and develop strategies to address our customers’ needs. Our mission: To ensure that patients receive the care they need, at a cost that makes sense for the healthcare system.
Every year we evaluate the top 10 trends in healthcare. The trends on this year’s list (below) are largely the same as they were 13 months ago, but COVID-19 has accelerated, intensified and amalgamated some of these trends in significant ways. This is likely to have long-term impacts for how healthcare is delivered in the future.
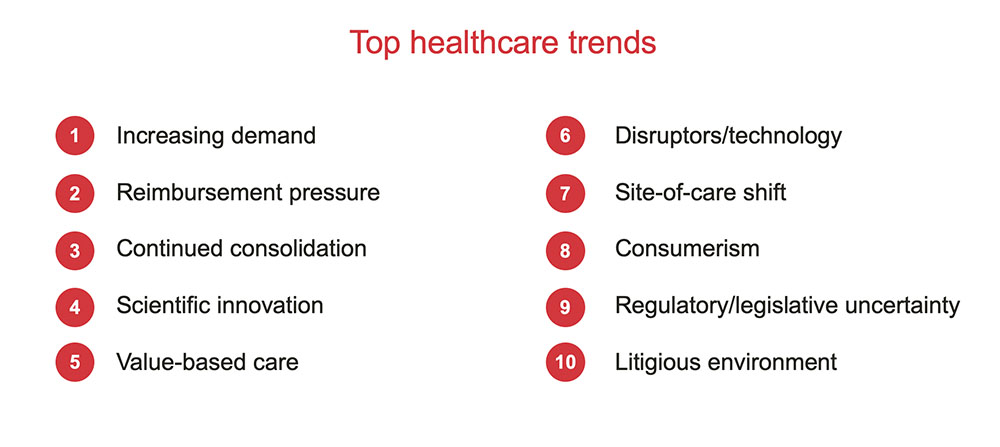
Some of the most meaningful accelerations I’m seeing are in three areas: patients are becoming more proactive in their own healthcare, providers are taking a more holistic approach in treating patients and the digitization of healthcare is enabling new treatments and determining the right treatments.
Patients are becoming more proactive, shifting sites of care
Patients are doing more research to understand, participate in and advocate for their own health. More than a third of us go online to identify and understand a medical condition. Although two-thirds of us say that looking up our symptoms online is overwhelming, we can’t seem to stop. Last year, each of us spent about a week of our lives looking for healthcare information online.
I believe that soon we all will expect to easily access medical information about conditions and payments online, just like we access the information in other parts of our lives. As this trend progresses, health systems, physicians, pharmacies, payors and other healthcare players will need to reconsider how they reach out to patients and share the medical information that informs patients’ choices.
The desire to advocate for our own healthcare is, in part, shifting where we get care. Even before the pandemic, healthcare was shifting from traditional acute care settings (hospitals) to more non-acute settings. Hip and knee replacements, for example, now often happen at ambulatory surgery centers rather than in hospitals.
The use of telehealth is accelerating – a trend that began several years ago. When the pandemic shut down physician offices, both patients and providers were pushed into trying telehealth as a solution and both became more comfortable with telehealth. And while the usage as a percentage of visits has normalized a bit, the jump seems to be “sticking” at around 10 percent of physician visits, compared to less than one percent prior to the pandemic. I anticipate that telehealth usage will continue to grow beyond the pandemic, potentially at a higher rate of growth than before the shutdown.
Another shift is an increase in home-based healthcare, including the delivery of medical supplies directly to patients’ homes. The use of “hospital-at-home” care, where patients are set up with hospital-like support in their own homes, increased 10-fold in the last year.
This shift, enabled by technologies like remote-patient monitoring, is being tested by many large health systems. Remote patient monitoring is also being used to run remote clinical trials. We expect to see more of this home-based care, as technology enables even better monitoring and response, resulting in better care.
Both physicians and health systems should assess how to respond to these trends, including what patient-interactions should occur using telehealth, and how hospital-at-home can be used to extend available bed capacity.
More consumers are accessing online pharmacies. With consumers taking so much of their care into their own hands, it’s no surprise that online pharmacies are growing. The online pharmacy market in North America was estimated at $31 million in 2020. The entire pharmaceutical market is about $300 billion in revenue, so there’s still plenty of room to grow. It will be interesting to see if patients further embrace online pharmacies and make this a dominant channel, or if online pharmacies remain a helpful but niche resource.
Increasingly, patients have the education and the tools they need, and the willingness to use them. They demand more from their healthcare providers, payors and suppliers. The real question is whether patients will have the patience to wait for the traditional healthcare system players to catch up to their expectations, or will they look to disruptors like Amazon to transform the healthcare space.
Providers are taking a more holistic approach in caring for patients
Social determinants of health and their close connection to racial inequalities in healthcare have been thrust into the spotlight as we wrestle with both the pandemic and racial justice issues. For some time, researchers have considered social determinants – including factors like access to food or pharmacies, the characteristics of a physical and community environment, economic stability and access to the healthcare system – as important contributors to a person’s health.
During the pandemic we have seen the dramatic impact of these inequities on people of color in our country. It’s a stark reminder that our healthcare system has systemic issues to address – in line with those that our society must address – with a more holistic approach to treat the person and achieve a more equitable set of outcomes.
We must learn from this pandemic and from other evidence of the disparities around us, to address the need for change and to design more effective solutions for all people.
Caregivers are connecting mental health with physical health. The pandemic has also greatly increased stress and anxiety for all of us, old and young, men and women. One in four older adults (65+) report anxiety or depression. Mental health-related emergency visits are rising significantly, both in younger children (ages 5 to 11) and in tweens and teens. And 83 percent of women, vs. 36 percent of men, are reporting significant increases in depression.
As the leader of Cardinal Health’s women’s employee resource group, I’m especially concerned about this last statistic. We know that women often play the role of Chief Medical Officer in our families, and if women are feeling the impact of depression and stress, how much more difficult will it be for them to fulfill that critical role?
What’s exciting, though, is that employers and payors are focused on mental health now like never before.
This shift implies a real need for healthcare organizations to work differently in how they look at the needs of their patient groups, then design and execute programs that address social determinants of health and both mental and physical healthcare needs.
Patients’ futures will surely be brighter, as employers, payors and providers drive toward improving outcomes, mentally, physically and across the spectrum of our communities.
Digital acceleration is unlocking advancement faster than ever
Venture funding is skyrocketing. Almost $10 billion were invested in digital health last year; in the first quarter of 2021 alone, investments reached $7.2 billion. Fierce Healthcare recently reported the 10 most interesting deals in digital health, which range from multi-billion dollar deals to small but potentially game-changing acquisitions of tech assets.
Healthcare is turning to predictive analytics. About half of healthcare organizations are now using predictive analytics; most believe that analytics can reduce costs by more effectively matching treatment decisions to patients’ needs: Who needs more care? Who can be treated at home? Who benefits from resources focused on social determinant issues?
Artificial Intelligence (AI) is transforming healthcare. The verdict is in: AI and predictive analytics are playing a role in transforming healthcare. AI empowers such things as precision medicine, medical imaging and drug discovery, and makes highly personalized therapies possible. The healthcare AI market is expected to exceed $34 billion by 2025.
This acceleration, driven in part by the pandemic itself, can drive our system to become both more efficient and more effective. We must find ways to harness this digitization, and bring together the vast quantities of data, modern analytics tools and a willingness to make changes. Healthcare data and technology can drive us toward a healthier world, with greater access and consistency in care for everyone.
All of this leads me to my conclusion that the future of healthcare is bright. The three key drivers – proactive patients who demand more, a holistic approach to healthcare and digitization – are coming together to create a flywheel effect, each driver building on the others to create a system that serves patients better and more cost effectively, and achieves better outcomes for all.
Michele Holcomb is the Executive Vice President, Chief Strategy & Business Development Officer at Cardinal Health. She leverages an enterprise perspective to work with leaders across the Pharmaceutical and Medical segments to define strategies and identify opportunities for growth in the evolving healthcare landscape. Her team also supports the execution and integration of innovation and acquisitions, partnerships and divestitures to support Cardinal Health strategy. Holcomb is a member of the board of Kimball Electronics Inc, Vineti Inc., Rev1 Ventures, and New Jersey’s Liberty Science Center. She sits on the Editorial Advisory Board of Pharmaceutical Executive, and she leads the Women’s Impact Network at Cardinal Health.
This post features highlights from a presentation Holcomb gave recently at The Future of Healthcare at The Ohio State University. You’ll find a recording of the program here.